Leah Pope, PhD, Senior Research Fellow, Vera Institute of Justice
David Shern, PhD, Senior Public Health Advisor, National Association of State Mental Health Program Directors
This article is part of a three-part series on how the criminal justice system can play a role in shortening the duration of untreated psychosis for people with mental illness who have become justice involved through the lens of the Sequential Intercept Model. Part one examines Intercepts 0 – 1. Part two examines Intercepts 2 – 3. Part three examines Intercepts 4 – 5.
The criminal justice system can play a central role in reducing the morbidity and disability of first episode psychosis (FEP). First episode psychosis is the first onset of a condition affecting a person’s thoughts and perceptions, which sometimes results in a mental health crisis. Law enforcement officers are often present at mental health crises. When they are trained in the knowledge, attitudes, and skills necessary to best to resolve these crises and refer people to appropriate community care, they can help provide optimal outcomes for both law enforcement agencies and the person/family in crisis.
During the last 5 years, there has been dramatic growth in the availability of evidence-based, specialty programs for persons experiencing a first episode of psychosis. Stimulated in part by new funding through the Substance Abuse and Mental Health Services Administration’s mental health block grants, new Coordinated Specialty Care (CSC) programs have been developed throughout the U.S. (see https://www.samhsa.gov/esmi-treatment-locator). CSC programs are team-based approaches that include recovery-oriented clinical support; educational and employment services; family support; and substance use services, with a strong emphasis on consumer engagement. Funding for these programs resulted from the effective dissemination of the National Institute of Mental Health (NIMH) Recovery After an Initial Schizophrenia Episode (RAISE) trial results. RAISE documented the effectiveness of the CSC program model in improving outcomes for persons with FEP. Adoption of the CSC model came alongside the increasing realization that many of our current mental health systems are not equipped to respond effectively to individuals with severe mental illnesses until these persons have developed significant disability related to their illness. CSC fills an important treatment gap in public mental health services by responding early in the trajectory of someone’s illness.
A key component of the CSC model involves extensive outreach by the CSC program to individuals or groups who are likely to have early contact with persons experiencing FEP. Shortening the duration of untreated psychosis (DUP) is essential to maximizing program benefits (e.g., reduction in symptoms and improved quality of life), so early detection, prompt referral, and linkage are key. School personnel, primary care physicians, law enforcement, family members, and clergy, in addition to the mental health specialty sector, form a network of early detectors who can shorten the DUP.
FEP and the Sequential Intercept Model: Intercept 0 and 1
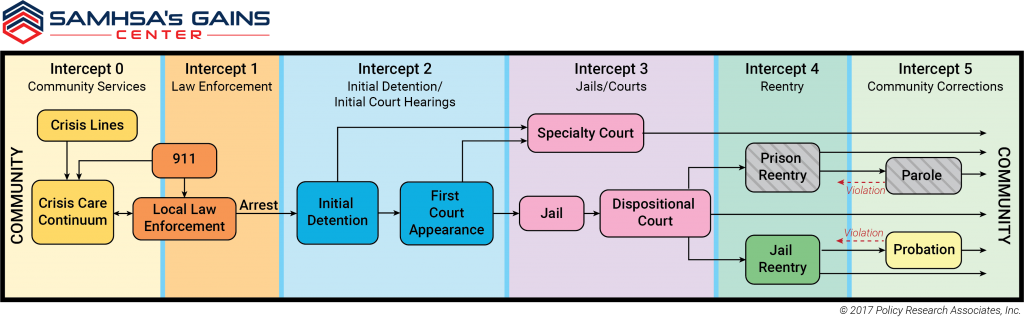 The Sequential Intercept Model (SIM) is a conceptual framework for understanding how people experiencing mental health crises may come into contact with and move through the criminal justice system. Intercepts 0 and 1 of the SIM are the first two intercepts where first responders and law enforcement may come into contact with persons experiencing FEP, as is depicted in the SIM graphic below. [For more information on the SIM, readers may refer to Policy Research Associates here].
The Sequential Intercept Model (SIM) is a conceptual framework for understanding how people experiencing mental health crises may come into contact with and move through the criminal justice system. Intercepts 0 and 1 of the SIM are the first two intercepts where first responders and law enforcement may come into contact with persons experiencing FEP, as is depicted in the SIM graphic below. [For more information on the SIM, readers may refer to Policy Research Associates here].
Intercepts 0 and 1 represent the earliest intervention points and highlight opportunities for collaboration among law enforcement and mental health and substance use treatment providers that can prevent deeper involvement in the justice system. These intercepts involve the behavioral health crisis continuum as well as first responder systems, including emergency medical personnel, fire fighters, law enforcement officers, and other first responders. The behavioral health components of the intercepts (e.g., crisis lines, mobile crisis teams, and crisis respite) represent the short-term crisis response models that are designed to identify and support individuals in crisis. Law enforcement responses, meanwhile, bridge Intercepts 0 and 1 to reflect how first responders, especially the police, have dual roles of preserving public safety and providing support to vulnerable individuals. Intercept 0 was recently added to the sequential intercept model to “more accurately reflects the collaboration and interdependency necessary for the crisis care continuum and law enforcement agencies…” to effectively serve persons experiencing a behavioral health crisis (Abreu, Parker, Noether, Steadman, & Case, 2017)[i].
Crisis Intervention Teams (CIT) are one example of a specialized law enforcement response that has been replicated nationally to respond to people in crisis and prevent arrest when possible. CIT is a collaborative strategy with multiple components, the best known of which is a 40-hour training designed to educate officers on the signs and symptoms of behavioral health conditions and to instill in them the knowledge, attitudes, and skills they need in order to intervene safely and effectively link individuals with care. Other forms of police-mental health collaborations are also being integrated in communities, sometimes in combination with CIT. For example, some agencies have co-responder models where a trained officer and mental health crisis professional respond together to mental health calls; others are implementing case management teams where behavioral health professionals and police officers collaborate to provide outreach to repeat callers and high utilizers of emergency services.
To the degree to which individuals in crisis exhibit psychosis, crisis care responses and police-mental health collaborations should provide immediate assistance and establish linkage with a CSC program (if one is available), which will reach out to the individuals and invite them to be assessed for appropriateness for the CSC program. Under circumstances in which a CSC program is not available, the crisis response team should link the individual with ongoing clinical services that are most appropriate for their needs and that maintain a strong consumer engagement and recovery focus.
Given the importance of decreasing the DUP and the likelihood that persons in crisis may encounter crisis response teams or police officers in the community, it is important for clinicians and criminal justice practitioners to collaborate and enhance opportunities for care coordination and linkage to CSC programs. Strong collaboration can ensure that people who interact with community crisis systems and law enforcement have clear pathways to CSC, and such collaborations have the potential to improve both clinical and legal outcomes for individuals with FEP.
With SAMHSA sponsorship, the National Association of State Mental Health Program Directors has worked with content experts to develop a portfolio of technical assistance materials. These materials are varied in their format and in the audience they target. (See https://www.nasmhpd.org/sites/default/files/Overview_Links_All_FEP_TA_Products_9-28-18_0.pdf for a brief description and links to all of the products.) Among these products is an issue brief that was developed specifically for the criminal justice system (https://www.nasmhpd.org/sites/default/files/DH-First-Episode-Psychosis-Considerations-Criminal-Justice-rev3_0.pdf). It provides basic information about psychosis and the CSC model and uses the SIM to discuss the settings and ways in which the criminal justice system can become a key part of the referral and detection network.
[1] Abreu, D., Parker, T., Noether, C., Steadman, H.J. & Case, B. (2017) Revising the paradigm for jail diversion for people with mental and substance use disorders: Intercept 0. Behavioral Sciences & the Law, 35(1), 1-16.


