The GAINS Center is supporting solutions for the urgent need to expand access to medications for opioid use disorder (MOUD) treatment in state prisons. Despite a high prevalence of opioid use disorder (OUD) among individuals with criminal justice involvement and the significant risk of overdose upon their release from custody, provision of MOUD in state prisons is limited. In a study of states with high levels of opioid overdose deaths, 61 percent of state prisons studied did not provide any form of MOUD.
Challenges Facing State Prisons
The effectiveness of buprenorphine, methadone, and naltrexone as MOUD is well established, and individuals who are taking legally prescribed MOUD are protected by the Americans with Disabilities Act. However, providing MOUD in state prisons is challenging for several reasons:
- Stigma around MOUD treatment persists among correctional staff, clinical and medical staff, probation and parole officers, and even individuals with OUD and their family members. Understanding that OUD is a chronic disease, rather than a personal choice, is associated with more positive attitudes toward MOUD.
- Policies and procedures for administering MOUD and deterring diversion for use other than prescribed should be clearly established and understood by all prison staff to address security concerns. Roles and responsibilities should also be formalized and clearly communicated. Developing this documentation requires up-to-date knowledge of statutes and regulations for MOUD dispensing and insight into best practices in medication administration among facilities of like size.
- The revised 42 CFR Part 8 rule requires seamless integrated care throughout the treatment continuum, which is critical to individuals receiving MOUD who are preparing to reenter the community from custody. Such care is highly dependent on careful planning and effective relationships with community-based providers, the State Opioid Treatment Authority (SOTA), and Medicaid, among others.
Federal Efforts Supported by SAMHSA
A series of SAMHSA sponsored listening sessions on promoting MOUD in carceral settings revealed the extent to which state departments of corrections (DOC) are struggling to expand access to MOUD for individuals in their custody. As a parallel effort to the Bureau of Justice Assistance’s work in expanding MOUD in jails through its Building Bridges Initiative, SAMHSA launched the Policy Academy on Advancing Medication for Opioid Use Disorders in State Prisons to accomplish the following:
- Foster shared values and a common vision for treatment of OUD in prison settings.
- Create a structured learning community for advancing policies and practices to implement MOUD.
- Develop relationships among multiple interested parties to advance state efforts to implement MOUD.
- Discuss insights, challenges, and opportunities related to implementation, continuity of care, and sustainability of MOUD.
- Create a strategic action plan for implementing or expanding MOUD in state prison settings.
 State teams selected for this ongoing initiative host an in-person site visit for GAINS Center representatives to introduce team members and relevant state-level leadership, and to identify key areas to address in the state implementation plan. This strategic plan is developed during a 2-day Policy Academy meeting, which includes facilitated working sessions and educational plenary sessions on core topics that inform the working sessions. Practical strategies are also provided to Policy Academy participants through technical assistance, including issue-specific consultation, webinars, and printed materials.
State teams selected for this ongoing initiative host an in-person site visit for GAINS Center representatives to introduce team members and relevant state-level leadership, and to identify key areas to address in the state implementation plan. This strategic plan is developed during a 2-day Policy Academy meeting, which includes facilitated working sessions and educational plenary sessions on core topics that inform the working sessions. Practical strategies are also provided to Policy Academy participants through technical assistance, including issue-specific consultation, webinars, and printed materials.
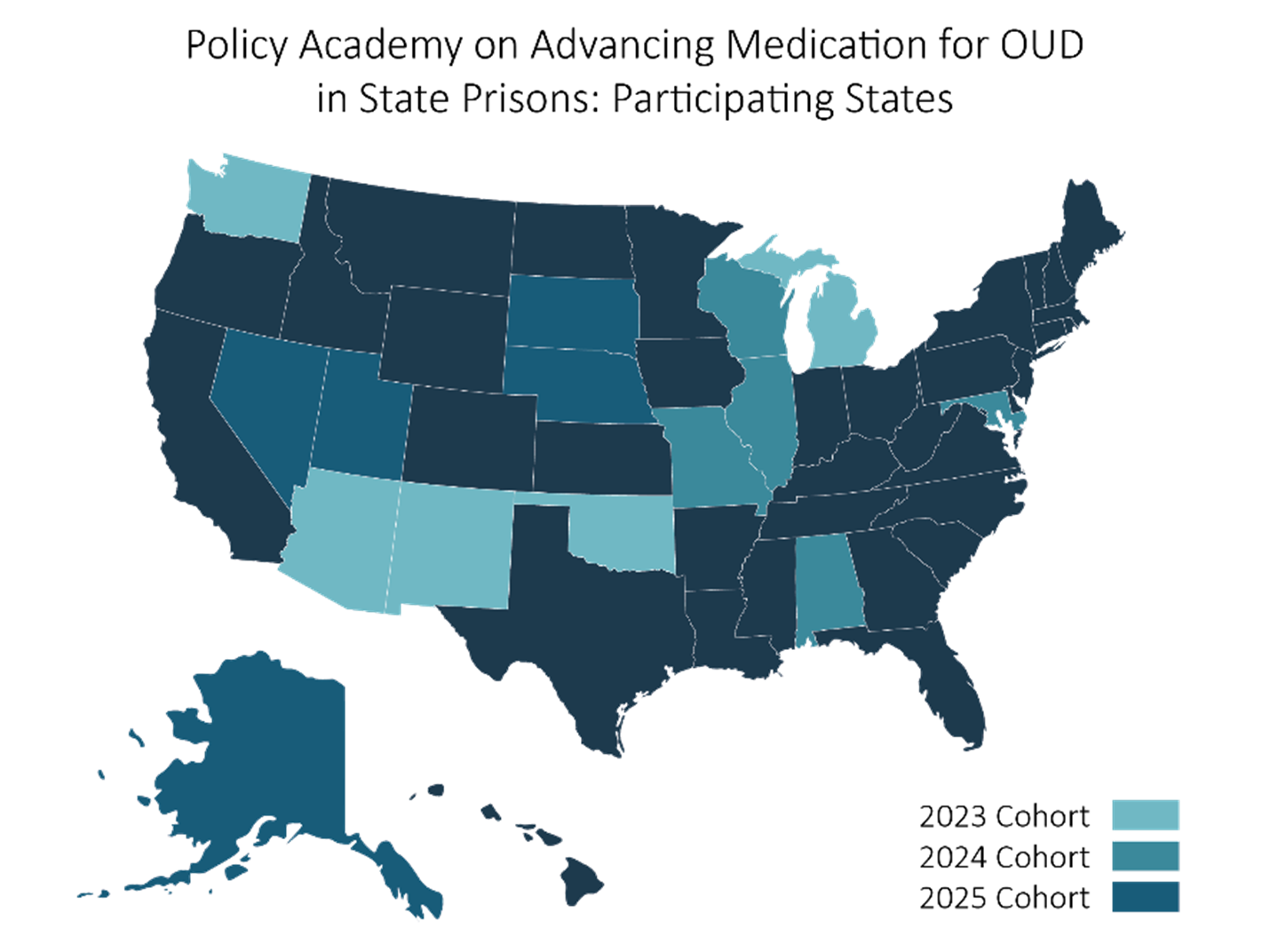
The Policy Academy has brought together 15 state teams in 3 unique cohorts. “We intentionally created cohorts to maximize peer-to-peer collaboration,” explains Shannon Bader, PhD, senior project associate. “By that, I mean providing an opportunity to discuss with and learn from other states in similar situations. In the first year, all participating states were essentially at the same place in the implementation process. Second-year cohort members represent DOCs overseeing a large prison population. Their challenges are quite different from DOCs with smaller prison populations, who make up the current cohort.”
To foster buy-in from key leaders, each state team includes a multidisciplinary group to ensure the involvement of correctional, medical, probation/parole, and state MOUD provision leadership. This is intended to support effective implementation of MOUD “behind the walls” and seamless continuity of care upon reentry. Participating states have included a mix of the following roles on their teams:
- Classifications administrator
- MAT/MOUD program administrator
- Medical director
- Addictions treatment director
- Reentry services director or manager
- Substance use disorder treatment director
- Mental health treatment provider
- Warden
- Custodial staff member
- Person with lived experience of incarceration in the state’s prison system
- SOTA
- Single state-agency representative
- Evaluator
- Legislator or legislative liaison
- Tribal leadership
- State Medicaid representative
Major Themes in Working with State DOCs to Implement MOUD
Intra-State Partnerships & Collaboration
“Seeing new connections take root has been one of the most exciting outcomes of this initiative,” observes Melissa Stein, DrPH, senior project associate. “For some teams, parole/probation had never been ‘at the table’ to talk about MOUD implementation behind the walls before the Policy Academy. Likewise, the SOTA, who is responsible for community-based treatment, was unknown to some of our participating teams before the Policy Academy.” Equally important has been the growth of partnerships and collaborations within the DOCs that may not exist or may be strained due to limited time for regular meetings. In many states, substance use treatment programs, addictions treatment providers, and mental health treatment are siloed. Furthermore, there is often little formal collaboration between medical and correctional staff (e.g., integrated policies, regularly occurring meetings, information sharing). In short, it is important that state DOCs have structured time and space to develop collaborations within their departments and across other state departments to ensure the success of substance use disorder (SUD) treatments in carceral settings.
The partnership-building work of the Policy Academy inspired a national webinar entitled “Medications for Opioid Use Disorder in Criminal Justice Settings: Developing Partnerships between Correctional Professionals and Community-Based Providers.” It speaks to the importance of working relationships between DOCs and community-based providers, and spotlights success stories, such as one DOC’s discovery of peer-run organizations willing to pick up individuals upon release from custody, which is a critical issue in rural areas with limited public transportation.
Cultivating Buy-In Among All Staff
Stigma and a lack of understanding about the nature of substance use disorders and MOUD treatment continue to be a challenge across most states. The Policy Academy initiative has clarified how important it is to educate correctional staff on substance use disorders, OUD, and MOUD, as well as on the policies and procedures for administering the medications. Correctional officers often view their work as following the commands of their higher leadership; thus, educating those officers on MOUD may be overlooked. However, state DOCs can make tremendous strides in fostering buy-in for MOUD and increasing the likelihood of successful implementation by investing in training their correctional staff on these medications.
Medical staff should also be prioritized for training as they may not have received any education about MOUD during their medical training, or the provision of MOUD may have advanced since their formal training. Stigma is also an ongoing challenge among clinical providers, so it is imperative that those staff also receive critical education about the nature of addiction and how to keep people experiencing SUDs alive using evidence-based treatments.
Medication Diversion
In some prisons, medication diversion may result in disciplinary discontinuation of MOUD treatment, but it is not medically safe or legal to deny treatment due to an infraction. Using a model policy on medication diversion, some states have received support in crafting medication diversion policies and procedures to keep discipline and consideration of treatment discontinuation separate. Clarifying the importance of holding people accountable for medication diversion using appropriate sanctions without withholding lifesaving treatment has emerged as an important focus of this work.
Staff Wellness
An unexpected outcome of the initiative addresses the historical struggle prisons have with adequate staffing, which was exacerbated by the COVID-19 pandemic. MOUD programming, especially at launch, can be labor-intensive, and adding another task to the workload can be daunting to staff members. This can be mitigated through education on the nature of substance use disorders, benefits of MOUD, and the legal argument for providing MOUD in prisons. But in addition to being informed, staff need to feel supported. To that end, Ronald Taylor, the chief of prisons at the National Institute of Corrections (NIC), presented a session on staff wellness at the 2024 Policy Academy. More information and resources may be found on the NIC’s Wellness for Corrections and Supervision Professionals webpage.
Stein comments, “Normalizing care—whether avoiding burnout as a staff member or receiving MOUD while in prison custody—is one of our goals. This work continues to transform facilities due to the federal government’s commitment to providing technical assistance well beyond the Policy Academy meeting. We’re eager to see how the momentum generated by these states will impact the national landscape.”
Culture Change
The emphasis on staff wellness was part of a larger conversation about the need for change in the traditional culture of corrections, which has historically focused on punishment and restrictions. Evidence is emerging about how the traumatic environment of prisons can adversely affect the physical and mental well-being of both incarcerated individuals and staff, long after the person has left the environment. Specifically, violence and the use of solitary confinement are two “norms” of prison culture that are being challenged. The work to implement a life-saving treatment for OUD has highlighted the greater need for a shift in the culture of corrections to provide treatment, foster healing, and support positive integration into communities post-release among individuals who often come into prisons with previous trauma and challenges.
Federal Requirements & Regulations
Finally, another major theme in supporting the DOCs was the challenges that state departments face in parsing both state and federal regulations to provide MOUD in the many facilities across their states. State DOCs navigate multiple competing priorities every day, from updating their “OMS” (Offender Management System), to implementing electronic health records, to responding to everyday incidents and medical emergencies. The expectation that they should also find time to parse complex, interrelated, and mandatory federal and state regulations related to MOUD provision can be a significant hurdle in implementation. One unexpected advantage of the Policy Academy work has been the support it has provided states on this topic, providing access to guidance and interpretation of regulations from federal agencies. The Policy Academies have also built awareness of the following existing resources to support DOCs in understanding and implementing MOUD in adherence to federal policies and regulations:
- Federal Guidelines for Opioid Treatment Programs (2024) | SAMHSA Publications and Digital Products
- Statutes, Regulations, and Guidelines for Medication-Assisted Treatment | SAMHSA
- 42 CFR Part 8 Final Rule | SAMHSA
- 42 CFR Part 8 Regulation Video Series: Snapshots for Implementation | SAMHSA
- Dear DEA Registrant | U.S. Department of Justice Drug Enforcement Agency (DEA) Diversion Control Division
- DEA Diversion Control Division Guidance Document | DEA
- Practitioner’s Manual: An Informational Outline of the Controlled Substance Act | DEA
- Narcotic Treatment Program Manual: A Guide to DEA Narcotic Treatment Program Regulations | DEA
- Guidelines for Implementing Medications for Opioid Use Disorder Treatment in State Prisons I SAMHSA
More Resources
- MAT Inside Correctional Facilities: Addressing Medication Diversion | SAMHSA
- Medication-Assisted Treatment (MAT) for Opioid Use Disorder in Jails and Prisons: A Planning and Implementation Toolkit | National Council for Wellbeing
- Toolkit: Medications for Opioid Use Disorder | All Rise
- Use of Medication-Assisted Treatment for Opioid Use Disorder in Criminal Justice Settings | SAMHSA
For more information about the Policy Academy, contact Melissa Stein at mstein@prainc.com or Shannon Bader at sbader@prainc.com.


